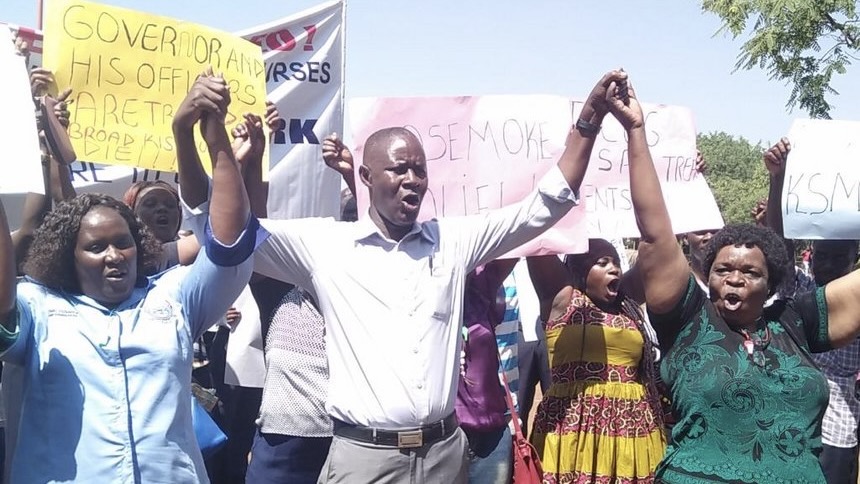At the end of October 2021, Human Rights Watch (HRW) issued a report warning about the dire state of health workers’ working conditions in Kenya. Otsieno Namwaya, East Africa director at HRW, said: “Kenya’s negligence regarding the safety and needs of health workers in the middle of a pandemic is completely unacceptable. Kenyan authorities should take urgent steps to ensure health workers on the front lines of the fight against COVID-19 are able to work in an environment that would not put them at unnecessarily heightened risk.”
Their warnings came after almost eight years of intensified industrial action by health workers in Kenya, shedding light on the turmoil they have been expressing. In the early 2010s, Kenya’s administration was structured through a devolved system of governance on two levels: national and county governments. Within the health sector, the national government’s role entails formulation of health policy and standards, and management of national referral services. The 47 county governments, on the other hand, hold health service delivery roles.
Ensuring that health care is available at the community level is of high importance in Kenya, as 65% of the 47.77 million population reside in rural areas. Unfortunately, this wasn’t secured by the devolution process, which has also meant that the provision of healthcare is split between public and private providers, making healthcare inaccessible to many.
Nurses on strike
For years, Kenya’s health system has experienced drug shortages, understaffing and underfunding. More recently, the system experienced three additional shocks: health workers’ strikes, devolution and the COVID-19 pandemic.
Health workers’ discontent and unrest seemingly coincided with the devolution of healthcare in 2013, with claims that the devolution process had been rushed and had resulted in challenges for health workers. Between 2010 and 2017, healthcare workers went on strike several times both on the national and regional levels, but returned to work with their concerns remaining largely unresolved.
In 2017, a 100-day doctors’ strike was followed by a 150-day nurses’ strike. Both strikes occurred because of the failure by the government to implement Collective Bargaining Agreements (CBAs) with their respective unions. While the long strikes ended, some issues have not been resolved: CBAs remained unsigned and the unions announced that the government should expect more strikes.
During the last year and a half, there have been new threats of strikes by health workers focused on grievances regarding adequate personal protective equipment (PPE), risk allowances and medical cover during the pandemic. Nurses in Kenya went on strike demanding immediate compensation of families of more than 18 nurses who had succumbed to COVID-19. Other demands included payment of $265 risk allowance to all nurses, confirmation of permanent contracts for nurses, free comprehensive medical cover for nurses for all ailments including COVID-19, and employment of 7,000 nurses to help fight COVID-19.
The strike went on for 79 days, and it included street actions in almost all county headquarters held on every Monday, media pressure, and slowdowns. The Council of Governors (COG) warned the striking health workers that their strike was illegal, and could result in mass layoffs. “No worker should expect to walk out of their jobs and then walk back when they so wish – the county governments are not a revolving door,” said COG Chairman Wycliffe Oparanya on this occasion.
Other health workers join in
In parallel to the KNUN strike, the Kenya Union of Clinical Offices (KUCO) went on strike for the same reasons. On this occasion, George Gibore, secretary-general of the KUCO, said: “The union has on numerous occasions raised concerns on the safety of health workers but the government has been adamant and always treated this advisory with contempt at the expense of increasing demise of health workers and other poor Kenyans.”
The Kenya Medical Practitioners, Pharmacists, and Dentists Union (KMPDU) also called for a nationwide strike over the 2017-2021 CBA and accused county governments of failing to implement the CBA, which sought to improve the working conditions for medics. Workers in public health facilities decried the provision of substandard face masks and other PPE. In some cases, health workers said the PPEs provided by county departments of health have been inadequate, forcing doctors to reuse them even during a pandemic. Doctors also condemned delays in payment of salaries by counties.
“Apart from delayed salaries in some cases for over two months in some counties, there has been a lack of commitment to address human resource issues including promotions. We are going to withdraw our services from the county hospital as soon as possible if our notice is not acted upon,” said Dr. Davji Bhimji Atellah, Secretary General of the KMPDU.
Ignoring health workers will further undermine the health system
The failure of the government to address the issues had a strong impact on the health care delivered. By not implementing the CBA for nurses, as well as classifying them as semi-skilled workers, only eligible for relatively low pay scales, the government fueled feelings of unfairness and under-appreciation among the health workers. Additionally, the lack of clarity and agreement between national and county levels on how to handle the strikes caused severe disruptions to health care delivery.
During the nurses’ strike, most dispensaries – primarily run by nurses – were closed, and many health centers ran on a ‘go-slow’ basis. Nurse-led services such as maternity, maternal child health and child welfare clinics were particularly affected, as well as community-based services coordinated by community health workers. During both the nurses’ and doctors’ strikes, there was a reported decline in hospital admissions and theater services given the interdependence across cadres at hospital level.
Outpatient services in public facilities sustained a decline during the nurses’ strike, as did inpatient admissions. This was linked to an assumption among community members that if one cadre was on strike, all facility services would be closed. Community members experienced difficulties accessing health care due to the time spent moving between public and private facilities, and negotiating initial deposits at private facilities.
The recurrence of strikes in the public sector in Kenya contributed to a loss of trust from the public in the public sector that might have longer term effects on treatment-seeking and the public health system. It is crucial the government addresses this issues by providing adequate working conditions to health workers.
Read more articles from the latest edition of the People’s Health Dispatch and subscribe to the newsletter here.
Dan Owalla is a paralegal and health activist in the People’s Health Movement Kenya circle.