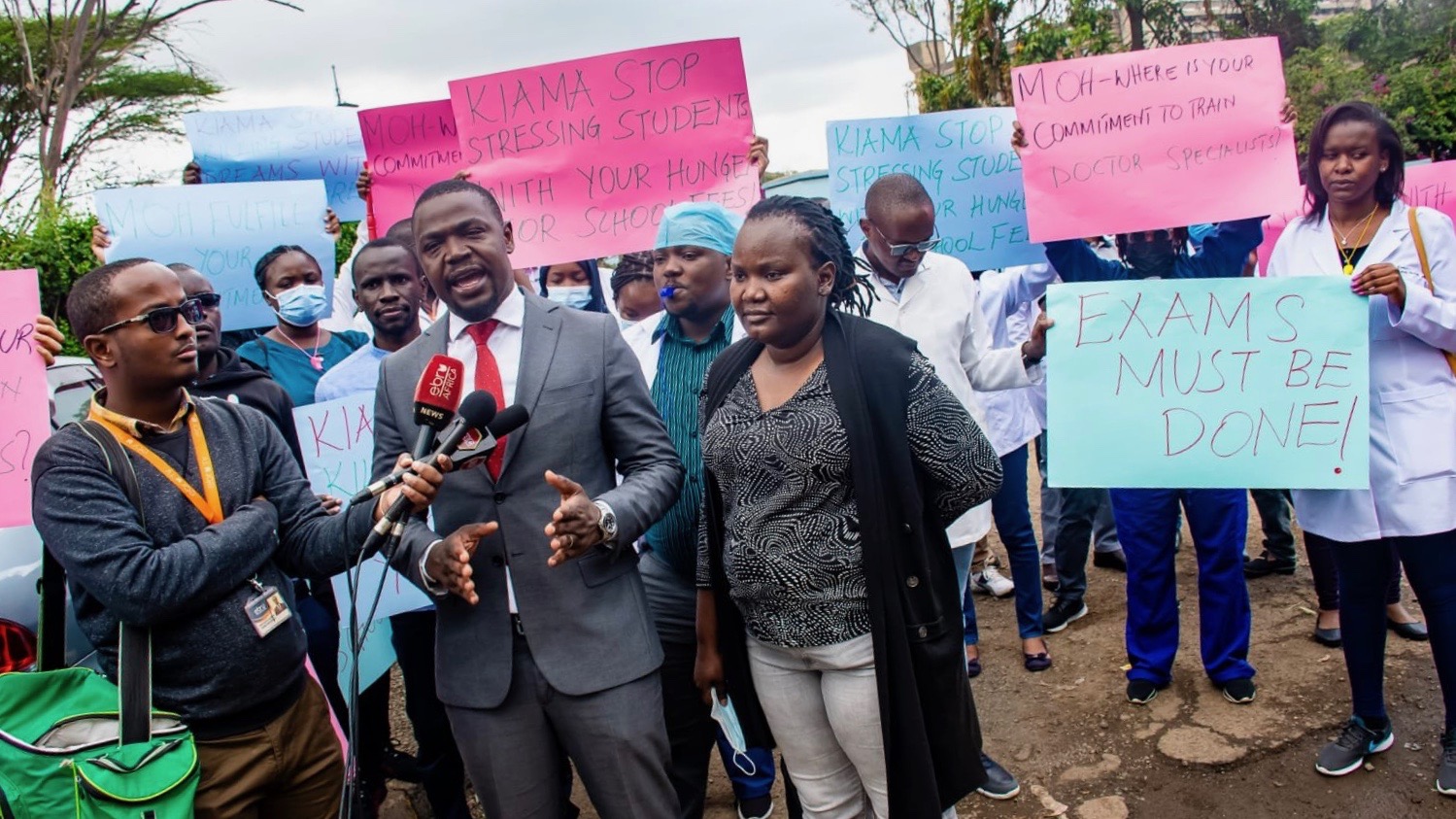In December 2022, doctors in Kenya warned they will go on strike if the government doesn’t address their concerns about a collective bargaining agreement signed in 2016. The agreement was supposed to address key health-related concerns in Kenya’s 47 counties, including problems with accessing essential medicines and referrals, but ended up being shelved as a result of the COVID-19 pandemic.
Dr Mercy Nabwire from the Kenya Medical Practitioners, Pharmacists, and Dentists Union (KMPDU) met with the People’s Health Dispatch to explain the reasons behind the health workers’ unrest, the obstacles standing in way of unionizing doctors in Kenya today, and building networks with right to health organizations and patients.
People’s Health Dispatch (PHD): Recently, doctors in Kenya warned they were ready to strike in case the government did not consider their demands for fair working conditions and the strengthening of the health system. Can you tell us more about the context in which this warning was published?
Dr Mercy Nabwire (MN): The context goes back to 2016, when the unions signed a collective bargaining agreement with the government of Kenya. This agreement included many clauses that were intended for the benefit of the doctors, but also for the improvement of the state of public healthcare in the country.
The Ministry of Health signed the agreement and committed to implement it, but already in December of that year, it became clear that the government avoided the implementation. We went to court, sued the government, and the court ruled that we were in the right—the government had to implement the agreement as agreed.
At around the same time, we issued a strike notice notifying the government that we need to have a conversation about the issues with the implementation of the agreement. It’s good to remind people that the agreement was not only about our rights, but had a lot to do with the conditions of the public health system. Our work environment basically corresponds to the quality of services that are provided in public facilities, and, at that time, both of these things were far from good. We did not have enough drugs and other supplies in public hospitals. Our referral systems were weak. There was a lot of corruption in terms of who gets hired. There was a lot of nepotism in terms of who gets promoted. There was just a lot of dysfunction within the public healthcare system.
The government ignored our notice, so at the end we went on strike. It was a very long and protracted strike, and it received a lot of attention at the time. We also faced a lot of pressures: the public health sector literally collapsed, some doctors were even arrested and put into jail.
After more than 100 days of strike, the government came up with a matrix for the implementation of the collective bargaining agreement at different levels of the administration. The health system in Kenya is devolved, so it has to be implemented at the level of the government, that is the Ministry of Health, which is responsible for policy and training, but also at the level of the 47 county governments that are responsible for service delivery. Those county governments are most practically responsible for ensuring that services within healthcare facilities are accessible to all Kenyans who seek them.
PHD: After this matrix was devised, did the collective bargaining agreement actually get implemented? What was the situation with its implementation during the COVID-19 pandemic?
MN: Let’s start with the information that the collective bargaining agreement we’re talking about was supposed to cover the period between 2017 and 2021. But most of that time has been spent on a lot of back-and-forth between the different government levels about the agreement, and not on implementation. By July 2021 both the Ministry of Health and the county governments had failed to implement many of the aspects of the agreement.
We’re talking about the period that spans the peak of the COVID-19 pandemic, mind you. A lot of doctors were losing their lives because of issues with the health system. Our COVID-19 response was very challenging because we did not have adequate personal protective equipment and diagnostics in our facilities. We did not have adequate staffing, we did not even have adequate infrastructure to address the pandemic. It was thanks to the dedication of health workers that the patients coming to the hospitals continued to receive care.
It was at that time that we again called upon the government and invoked the clauses of the agreement that referred to their responsibility to ensure adequate staff, supplies, infrastructure, and medical insurance, to ensure that, if we fell ill, we would then not need to go into our pockets to pay for the very same care that we were providing. We wrote many letters to the government, did a lot of press conferences, just calling upon the government and highlighting the number of doctors we were losing, highlighting the inadequate facilities that we had in the country, and highlighting the lack of medical insurance.
We lost some doctors because they could not afford to pay admission fees to get admitted into the hospital. We lost them because of that. At that moment, the doctors said: “You know what? We are in the midst of a pandemic. This is very difficult for us. We are putting our lives on the line, but nobody seems to care. We are going to down our tools.”
The doctors went on a strike that lasted, I think, five days. During those five days, the government moved to court, of course, claiming that it is immoral for healthcare providers or frontline workers to go on strike during a pandemic. And at that time, the court suspended our action, but it also instructed the government again to go ahead with the implementation of the collective bargaining agreement. That was in 2020. By last year, the government had not done anything towards implementation despite the court ruling. Once again, we went to court, requesting it to issue fresh orders as well as protect any industrial action that we may wish to undertake to compel the government to address these issues. Again, the court instructed the county governments and the national government to implement what they had agreed to, and then to report back. But again, all of our attempts and demands were ignored, and by then it was already December 2021.
PHD: And after that, the formal period implementation of the collective agreement had ended. But did something change in 2022?
MN: That was an election year and there was a lot of attention given to that. You know, the story of the day was who was going, who was coming, what’s going to happen in general. There was really little activity to address the concerns of workers by those who were then holding office. Since that was the then President’s final term, we decided to wait until the end of the election to address our issues.
Parallel to that, we held our annual conference, which brings together almost 600 doctors from all around the country, each of them representing 20 more members of our union. Of course, the conference discussed all these challenges that we were facing, and it became clear to us that if we wanted to get the public health sector functioning in this country, we needed to make no other demands apart from the government implementing the existing collective beginning agreement—because it addressed various aspects of the health system that still needed strengthening. We agreed that rather than begin a whole new cycle of negotiations, we just needed the government to implement the collective bargaining agreement as it was.
The conclusion of that meeting was to issue a strike warning, in case the new government wouldn’t even begin to talk to us, to address, at least in some small way, the issues that we have. Issues of unemployment, inadequate supplies and drugs, issues of a weak referral system. These are problems that we have to deal with every day while pretending to work in a functional system. The truth is, the majority of us go to work to supervise death, and that is very sad.
We really want the government to come to the table and see how we can make things better. Just by implementing that collective bargaining agreement, you know, we could have a better health system. We could still have a motivated workforce, and we could ensure that the quality of care that patients in Kenya receive is of the highest standard that it can be.
Doctors issued that last strike warning because we are tired. We are not seeing any meaningful investment in healthcare in terms of budgetary allocation to the sector or reforms towards strengthening the devolved systems to address the unique challenges in the health sector. And what we have been seeing is also that the government is adamant. It was just adamant in not addressing healthcare as a priority for Kenyans.
It should be said that, before we issued the strike notice, we had various engagements with different organs of the government, different agencies. They have made certain commitments, so we agreed on a 60 day framework during which the government committed to implement certain things. We also have a mechanism in place that ensures that after every 15 days we are able to check and see if they are respecting the commitments they have signed on to.
PHD: From the story of the last six years, it really becomes clear how important trade unions can be for doctors as they fight to protect their rights. But what is the situation with actually organizing workers in the health sector?
MN: Let’s start by saying that before the 2010 Constitution, healthcare workers, including doctors, were not allowed to become members of a trade union or even participate in trade union activities because they were classified as essential or emergency workers. The new constitution allowed every single employee in Kenya, except for the armed forces, to become a member and participate in the activities of a trade union.
Now, at that time, we were able to organize ourselves and form the union, but initially there was some reluctance from certain sections, certain groups of doctors, to join the union. Especially the older doctors, because it was the younger doctors at the forefront of organizing the union. The recruiting was really taxing. We really had to be out there, convincing people it was important for them to join the trade union. This was also because although there were challenges in terms of employment at that time, they were not so obvious as later. Until 2016 or so, the government used to post doctors who had completed their training for internship, and after the internship they would be absorbed directly into the public health sector.
When the union came into existence, there was an improvement in the basic salary and in welfare. There was a little bit of structuring in the way promotions and training were being done. And, through that, doctors began realizing the importance of unionizing. That brought a big rise in the number of doctors joining the union. And I have the feeling that after the 2016 strike, every single doctor in the public health sector in Kenya wanted to join and actually joined the union.
From 2017 onwards, the government stopped the automatic employment of doctors post-internship. I’m not sure if it’s part of a strategy to weaken trade unionization among doctors or something else, but it happened. Now a doctor will complete their training, do their internship, and then after the internship they will have to go around the counties looking for jobs, and not get employed. We have a huge pool of unemployed doctors, and this has allowed both the county governments and the national government to employ doctors on a contractual, short-term basis. Often, one of the conditions to get that kind of employment is that they will not become members of a trade union and they will not participate in trade union activities.
This is making trade unionization very difficult, especially among the young doctors who really want to join the union, but are prohibited to do so through terms of their contracts. And the other terms are really bad as well, you know; sometimes they are even paid on a day-per-day basis. It’s like, today, you come to work in the morning, do your work, you get paid. Tomorrow we don’t need you, you don’t come, you don’t get paid. And we’re talking about highly specialized, highly qualified workers here—imagine what that says about work in other sectors.
PHD: Is there a way the union can still support doctors in these conditions?
MN: As a trade union, we engage with the employers saying: “We represent every doctor who is under your employment, and these are the terms of employment. We expect all doctors that you bring on board will be employed respecting these terms.”
The thing is, this kind of employment was encouraged by the COVID-19 pandemic as well. You know, they saw they needed more staff, so they employed doctors on short-term contracts to make sure there’s enough of them attending to the patients. But they also paid them minimum wage, not the same wage that the others were paid, because the resources they had at hand were not enough. They thought, “this is the little money that we have, so we’re going to distribute it amongst these doctors.” They didn’t think about how to increase the whole amount.
It’s not just doctors who started being employed on contract. We see nurses being employed on this kind of contract. We see clinical officers being employed on short-term contracts. And it is very short-term contracts, in the line of 3 months or so. After the three months, you are at the mercy of the county government.
We see this as an onslaught on the health workforce, because the rights of a young doctor who has just come out of school and is earning their salary on a daily basis are definitely not the same as those of a doctor who has been employed on a permanent, pensionable basis. This young doctor does not even have any medical insurance. If they fall ill, they’ll have to pay out of pocket for their care. If they do not show up to work, they do not get any sick leave. They do not get any annual leave.
But this kind of shift in employment practices is also an onslaught on the workers’ right to unionize and an onslaught on the trade unions in the sector. The trend is affecting all health cadres who have been able to unionize, and we have gone to court to invoke the Constitution and to challenge the practice, especially since it’s happening in a part of the workforce which is providing essential services.
As a union, we are also trying to become very flexible in terms of defining who is our member. We are not insisting that a member is only someone who pays the full membership fee, but we’re defining our member as a doctor who is employed in Kenya. No matter what the employment format, these are our members. Those are some of the things we are doing as a union to be able to continue to organize and push back on the precarization we’re seeing.
PHD: This is an interesting approach, also because we’ve seen governments around the world actually seize the COVID-19 pandemic as an opportunity to undermine the rights of health workers, although they were apparently applauding their efforts. Another thing they are doing is painting health workers’ industrial actions as opposed to patients’ interests. How successful have you been in avoiding that and building relationships with patients and right to health groups?
MN: We tried hard to connect to our patients in the run-up to last year’s election because we realize that they’re not just consumers of services that we as health workers provide. They’re not just patients, they’re also citizens of this country, and their health depends on many things. We took a very radical approach of politicizing healthcare and making sure that it becomes a talking point in the run-up to the election. We moved beyond engaging with only patients’ associations and partnered with a lot of community-based organizations, organizations that address issues related to healthcare.
And I don’t mean just health services or delivery, but also social determinants of health, other issues that affect quality of life and health, like access to water, sanitation, or climate justice. Providing education on these topics is as essential as discussing health delivery, because what we want to show is that a lot of the diseases we face could actually be prevented if the conditions were right. If we had a proper, strong primary health care system, we could do that.
Together with community-based organizations, especially in informal urban settlements, we do outreach programs. That means we go out into the communities that have difficulty accessing quality healthcare and we provide these services to them at no cost, while at the same time we demand from the governments in those areas to set up adequate health facilities. We do this to them to let people know that we are human, we care about them.
We also partner with organizations that do different kinds of advocacy, like the People’s Health Movement Kenya. With them, we did many campaigns to increase the uptake of the COVID-19 vaccine, to support the TRIPS waiver, to ensure a review of the health budget to consider pandemic preparedness. We also work with Amnesty International on their government assessment activities, where we are able to take up the health aspect of the scorecard and do a comprehensive assessment of how the government performed there.
Finally, we also work with community health volunteers and community health workers. These are workers that essentially make up the foundation of our sector, but they are very weakly represented and have little room for organizing. For the past two years, we have been working with community health workers and volunteers, first and foremost, just trying to federate them, trying to bring them together.
We have also sent memoranda to the Parliament and the Senate to have them recognized as workers in order to have their essential rights protected. That is something we are doing because, unlike the community health volunteers and the community health workers, we already have a platform from which we can speak. As the health workers with the highest skill set, if we can put it like that, doctors are able to knock on certain doors and these doors open. Not all health workers are in the position to achieve the same, unfortunately.
Through the link with community health workers and volunteers, we also connect with the patients that they work with. We have worked with advocacy groups among patients, including those living with cancer, who are trying to address the stress and suffering that arises because not all of their health needs are addressed. And this does not happen because of a health workforce that is unresponsive to people’s needs, but because the entire system is currently unresponsive to them.
People’s Health Dispatch is a fortnightly bulletin published by the People’s Health Movement and Peoples Dispatch. For more articles and to subscribe to People’s Health Dispatch, click here.